What are the Clinical Care Standards?
The Clinical Care Standards are a group of 17 evidence-based quality statements that address the expected level of care and outcomes when managing specific health conditions.
They include guidance for both clinicians and health service organisations, and also include expectations for consumers receiving the relevant type of care. Each Standard includes a set of indicators that can be used by health service organisations to support implementation, monitoring and identify areas for improvement.
The aim of the Standards is to set out a baseline standard of care for the delivery of clinical care wherever this care is being provided, and to reduce variation in care outcomes. Broad implementation of the Standards should ensure that:
- Patients understand the care they’ll be receiving in order for them to make informed decisions;
- Clinicians and healthcare professionals understand current best practice, and use this to inform their care delivery; and
- Health service organisations understand how to best support their clinicians and monitor the level of care their patients are receiving.
The National Safety and Quality Health Service (NSQHS) Standards, which must be followed by all public and private hospitals, day procedure services and public dental practices, include actions that support or require the implementation of the Clinical Care Standards.
Who should follow the Standards?
Two of the Clinical Care Standards, Antimicrobial Stewardship and Delirium, are explicitly referenced under Action 3.18 and Action 5.29 respectively of the NSQHS Standards. Compliance with the requirements of these Standards therefore forms a part of mandatory NQSHS compliance for health service organisations.
Advisory AS18/12 also mandates the Colonoscopy Clinical Care Standard for any health service organisation that provides colonoscopy services under Actions 1.23, 1.24, 1.27b, and 1.28a of the NSQHS Standards.
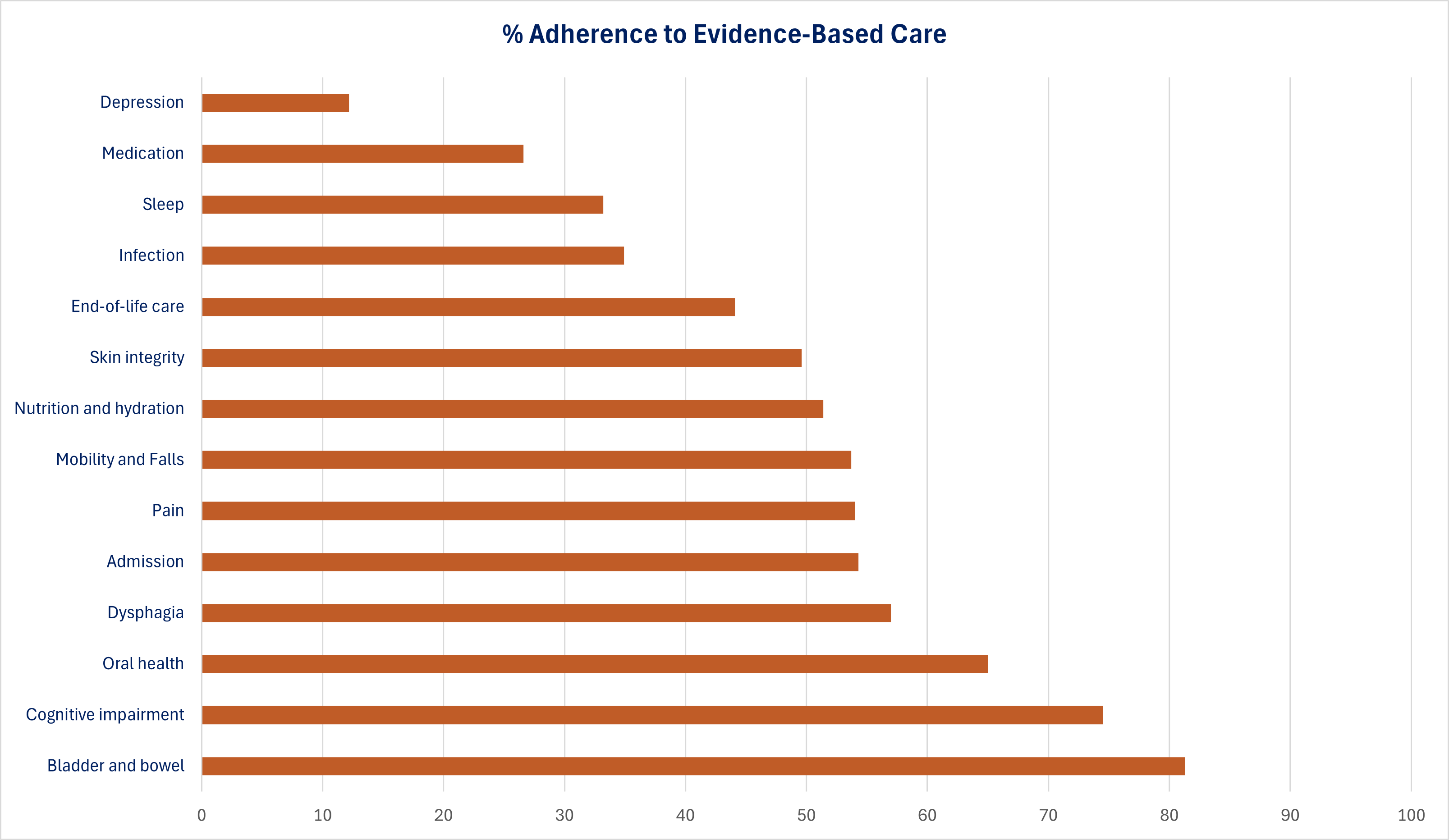
Following the Clinical Care Standards that are relevant to your service is strongly encouraged as best practice, as it supports improved outcomes for patients. An evaluation report of the impact of the Clinical Care Standards on patient outcomes revealed that 92% of health organisations surveyed who had implemented one of the Standards reported that it improved the quality of care delivered to patients in that care area. Secondary health data sources relating to the Antimicrobial Stewardship, Delirium and Hip Fracture Standards demonstrate a correlation between the release of each Standard and improved outcomes in the respective areas.
Implementation of relevant Clinical Care Standards can help organisations meet their obligations under the NSQHS Standards, in particular Actions 1.01c, 1.27b, and 1.28.
Which clinical care areas are covered?
The following areas have a specific clinical care standard:
- Acute Anaphylaxis;
- Acute Coronary Syndromes;
- Acute Stroke;
- Antimicrobial Stewardship;
- Cataract;
- Colonoscopy;
- Delirium;
- Heavy Menstrual Bleeding;
- Hip Fracture Care;
- Low Back Pain;
- Management of Peripheral Intravenous Catheters;
- Opioid Analgesic Stewardship in acute pain;
- Osteoarthritis of the Knee;
- Sepsis;
- Stillbirth;
- Third and Fourth Degree Perineal Tears; and
- Venous Thromboembolism Prevention.
In addition, the Australian Commission on Safety and Quality in Health Care is developing two new Clinical Care Standards, covering Chronic Obstructive Pulmonary Disease and Psychotropic Medicines in Cognitive Disability or Impairment. The Acute Stroke, Heavy Menstrual Bleeding, Osteoarthritis of the Knee, and Colonoscopy Standards are under review.
The Clinical Care Standards in SPP
A number of our health service clients asked us to look at developing self-assessments to implement some of the Clinical Care Standards. So we’ve worked with them to build one for the Antimicrobial Stewardship Clinical Care Standard, which is now available in SPP.
A self-assessment for the Delirium Clinical Care Standard is on the way next, so make sure to keep an eye out for it!
Organisations can use the results from completing each Clinical Care Standard as evidence to support their compliance against their NSQHS requirements.
If there’s a particular Clinical Care Standard you’d be interested in accessing as a self-assessment, we’d be keen to hear from you – just let us know!
Are you up to date with your NSQHS compliance?
Sign up to SPP to check how your organisation performs against the NSQHS Framework.